With the recent reports of Legionella in the news, many facility managers wonder if an outbreak could happen at their hospital. It can. The following environments in healthcare facilities offer the ideal environment for Legionella growth:
- Potable water system and outlets. These include the incoming service, water tanks, water softener, showers, and faucets.
- Cooling tower and condenser water systems, including chillers, the tower basin, and sump.
The heat and semi-inactive states of these settings, combined with their aerosolizing mechanisms (jets, sprays, and mists), make it possible for patients to inhale or aspirate contaminated water droplets. Although healthy people can contract this illness, hospital patients with compromised immune systems are most susceptible.
Water Controls to Maintain Temperature
Water systems with ambient temperatures that exceed 68°F are susceptible to Legionella growth. As are systems with prolonged periods of low flow or non-use. Thermal eradication heats water temperatures above 124 °F to inhibit bacterial growth. But, skin can scald at 110°F or burn at 140°F. Mixing valves at outlets prevent injuries by reducing the water temperature below 110°F just before it exits the system. Insulation, automatic drains, and recirculating loop distribution systems further regulate water temperatures.
Water Controls to Maintain Flow
Legionella bacteria grow in stagnant water. The engineering controls that maintain temperatures also must have the ability to regulate water flow. Knowing if your controls are capable of maintaining flow is difficult as the components that regulate flow are seldom visible. However, storage tanks and dead leg pipes capped during a renovation are common culprits. To prevent stagnation, water pumps should run continuously and remain separate from energy conservation programs.
Chemical Control
There is no guarantee that any water treatment can eradicate the organism. Instead, hospitals can prevent Legionella growth with oxidizing agents such as biocides or chlorine. Continuous chlorination, the method used for most cooling towers in the United States, is not an option for potable water systems. Hospitals must treat potable water systems with engineering controls that use temperature mitigation.
How to Proceed
Where should you start? While a water quality engineer tests for the presence of Legionella, a plumbing engineer identifies the infrastructural elements that foster Legionella activity.
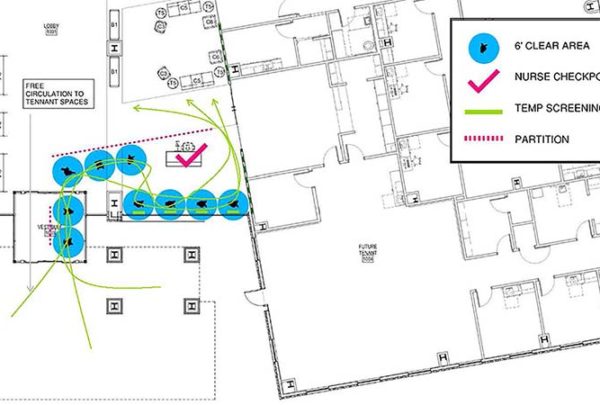
Plumbing engineers begin by performing an as-built survey to identify possible Legionella growth sources. Then, they recommend engineering controls to deter future bacterial cultivation. Any prevention measures they recommend should follow the latest guidelines: ASHRAE 188-2015.
Don’t be the next facility in the news. Rely on an engineering partner with expertise in healthcare facility plumbing infrastructure and distribution systems to assist you in this endeavor.